
Category: Research
 Category: Research |
| Teaching and Learning Forum 2014 [ Refereed papers ] |
Olivia Gallagher, Rosemary Saunders, Karen Tambree
The University of Western Australia
Selma Alliex, Leanne Monterosso
University of Notre Dame
Y. Naglazas
Bethesda Hospital
Email: olivia.gallagher@uwa.edu.au, rosemary.saunders@uwa.edu.au, karen.tambree@uwa.edu.au, selma.alliex@nd.edu.au, leanne.monterosso@nd.edu.au, ynaglazas@bethesda.asn.au
The Building Capacity in Palliative Care Clinical Training project commenced in 2012 and is providing a dedicated palliative care clinical learning experience for nursing and medical students as part of preparation for palliative care practice in future workplaces. Many students fear death on a clinical placement. This paper reports on a pilot study as part the broader project evaluation that examined nursing students' experiences of death and how the project driven teaching and learning supported students' learning experiences.
Palliative care clinical placements can be an overwhelming experience for the nursing student, presenting the individual with both personal and professional challenges. Adequate clinical experience in this area is fundamental to preparing health professionals for the workforce. Palliative care units in the past have not offered high numbers of student placements. There are many reasons for this including the often small size of palliative care units with low patient numbers and the demands of supervision in this vulnerable area (Mok & Chi, 2004).
The University of Western Australia (UWA) in collaboration with the University of Notre Dame Australia (UNDA) and Bethesda Hospital received funding through Health Workforce Australia to implement a project aimed at building capacity in palliative care clinical training. As part of the Building Capacity in Palliative Care Clinical Training project (http://www.meddent.uwa.edu.au/community/bethesda) nursing students undertake a clinical placement at Bethesda Hospital in the Palliative Care Unit and Palliative Ambulatory Service, providing various opportunities to work with the multidisciplinary team to participate in care delivery to palliative patients including assessment, symptom management and end of life care in accordance with the Australian National Palliative Care Guidelines. A dedicated Practitioner Scholar supervision model was implemented to provide consistent support and education to both nursing students and Bethesda Hospital staff during student clinical placements. The Practitioner Scholar is a palliative care nurse educator based in the clinical setting during student placement to support and facilitate student learning. An intensive ratio of 1 Practitioner Scholar to 6-8 nursing students was adopted.
A variety of teaching and learning strategies are used as part of the palliative care placement. Learning resources and supporting materials from the Australian Government's Palliative Care Curriculum for Undergraduate Project (PCC4U) are also utilised (Australian Government Department of Health and Ageing, 2005). Practitioner Scholar-led tutorials and discussions covering Principles of Palliative Care; Communication; Palliative Assessment and Intervention and Optimising Function in Palliative Care; student-led case based discussions and video illustrations of end of life scenarios are used as part of the teaching and learning. Students are allocated to the care of a patient (and their family) or group of patients receiving palliative care, and deliver the care in partnership with the health professional team under the supervision of a registered nurse. This pilot study exploring nursing student experiences of death and dying was an important first step in identifying nursing student learning needs and the support they required. Evaluation of the extent to which this project model prepared hospital staff and the Practitioner Scholar to meet these needs was also undertaken.
Of all deaths that students had experienced, 69.2% of students had been present when a person died. The deaths experienced by students were predominantly grandparents (84.6% of respondents), friends (61.5% of respondents) and patients (61.5% of respondents). While on clinical placement in the Palliative Care Unit of Bethesda Hospital, nursing students experienced between 1 and 20 patient deaths (mean= 5.5 patient deaths) in a 10-15 day period.
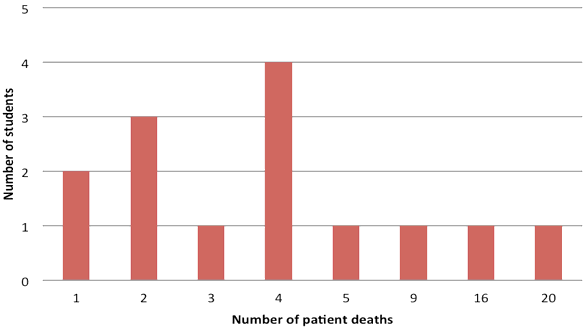
Figure 1: Number of patient deaths experienced by nursing students
while on clinical placement at Bethesda Hospital
Nursing students reported providing direct care to between zero and five dying or deceased patients (mean= two patients). Care provided to these patients were recounted to include emotional support (69% of respondents), pain management (50% of respondents), emotional and/or social support of the family (44% of respondents), assistance with activities of daily living (37.5% of respondents), and comfort measures (37.5% of respondents).
That in the lead up to the death, the patient has been made comfortable and pain has been adequately managed. That any final wishes/instructions they have given about this phase is upheld. That they are not alone as they pass, that either family or someone caring is present with them.Students' descriptions of a 'bad death' juxtaposed their perceptions of a 'good death', with the focus on being unprepared for death and trauma experienced by the patient and their family. Respondents describe a 'bad death':Patient dies in a comfortable manner. Their pain level should be at the lowest possible level, their physical, emotional and spiritual needs are considered and catered to. Patient and family should be educated about what to expect as patient declines. Patient is treated with respect and dignity.
Patient is in pain both physically and emotionally. When they have not come to terms with what is happening, have not put their affairs in order and when the family are not accepting.End of life care was commonly described using the terms 'providing comfort care' (N=8), 'supporting family members' (N=5) and 'holistic care' (N=3).A death which involves factors or interventions which are not consistent with the persons wishes and/or beliefs/values. Painful, traumatic- including trauma for the persons family.
Manage the symptoms and offer comfort for the patient with terminal illness, respect their right on decision making, protect their dignity and privacy, present physical and emotional support for both family and patient.End of life care refers to care provided for patients at the end stage of their disease where they have days to weeks to live. The physical, emotional and spiritual needs of the patient and their family is the primary focus.
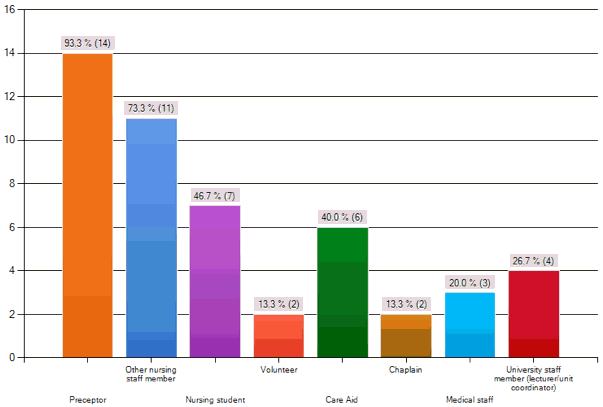
Figure 2: Role of persons who provided support to nursing students
Nursing students overwhelmingly agreed the Practitioner Scholar was supportive during their experiences of death and dying (N=15, 93.8%). Nursing students reported this support was received by the Practitioner Scholar always being available, providing education on palliative care and facilitating debriefing. Student responses to "How did the Practitioner Scholar support you?" included:
Always available to talk, offered support when she knew we had experienced death, gave (sic) us the opportunity to talk about our feelings, either in private or with other students.The single student who disagreed that the Practitioner Scholar was supportive stated they could have been more supportive by asking about past experiences of death before asking the student to assist with care of a recently deceased patient.Myself and the group of students on placement with me attended a daily session with the Practitioner Scholar where we discussed our experiences. She was always so available for one-on-one debriefing sessions if needed and she was very supportive in general.
Debriefing following a patient death on clinical placement in the Palliative Care Unit at Bethesda was provided to 80% of respondents. While all respondents who were debriefed reported being debriefed by the Practitioner Scholar, various other staff members and nursing students also facilitated debriefing of the nursing students as shown in Figure 3. Participants selected all that apply, as on some occasions multiple staff conducted debriefing. All nursing students who received debriefing found this helpful. Of those nursing students that were not debriefed (N=3), two agreed it would have been helpful to debrief, while one disagreed.
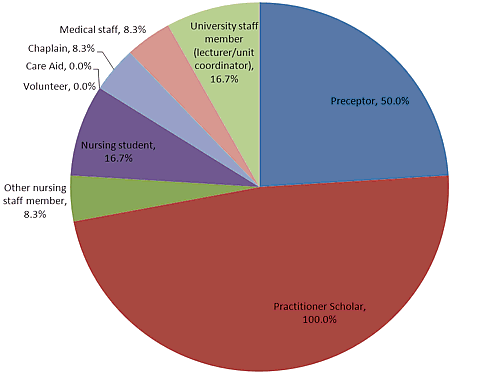
Figure 3: Role of the person/s who led the debriefing/s with the students
One hundred percent of nursing students reported sharing their experiences of death and dying with family, friends or fellow nursing students. The majority reported this as useful, however 7.7% were uncertain.
The lectures provided me with a general idea of what to expect when working in a palliative care unit. As a result of this I had an idea of some of the challenges associated with working in this area.The education sessions that were provided as part of the placement were also valued. Over 50% of all students reported attending all the education sessions, and over ninety percent attended the Principles of Palliative Care and Communication session. All students either agreed (40%) or strongly agreed (60%) that attending these education sessions was helpful and informative.It helped to clarify what palliative care was all about, and to give some idea of the types of experiences we may have.
I think general awareness of palliative care and death and dying are useful, since at some point in our careers we will have to deal with people who are suffering from life limiting illness and/or dying. Also useful is knowledge of the way in which care is delivered and respecting the patients wish to withhold treatments or medication. Communication is one of the other most important lessons I have learned; and how talking with the patient and their family is all part of good nursing care regardless of the setting you are working in.When asked which clinical settings respondents believed such skills, knowledge and experiences were transferable to, 57% identified they were applicable to any or all clinical settings. Other specific clinical settings identified included community, hospital, nursing home/aged care, critical care and oncology clinical settings.A deeper understanding of the dying process and how it affects the person who is dying and their family. Experience of providing care. An understanding of patient and family advocacy and a better understanding of when and how it might be appropriate to make a referral to a palliative care team.
Participants were asked to reflect on their interest in practicing in the area of palliative care as registered nurses. Responses were evenly dispersed between yes, no and maybe.
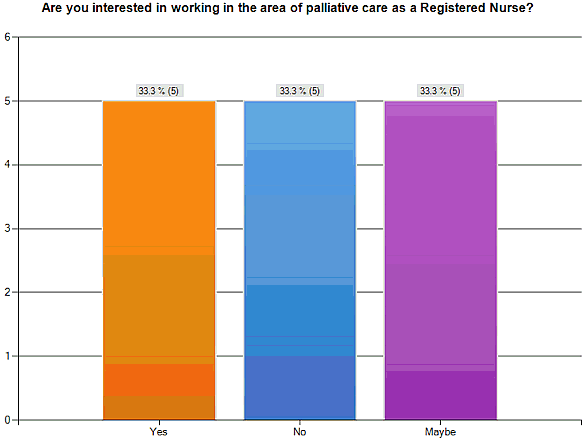
Figure 4: Student interest in working in palliative care as a Registered Nurse
The findings also indicate that, irrespective of previous experiences, nursing students' experiences of death on a clinical placement also caused them considerable anxiety and sadness. This finding is not unique as the experience of death and dying for nursing students and new graduates is reported as one of the most stressful experiences in nursing (Deffner & Bell, 2005). Nursing students in this study reported experiencing an average of 5.5 deaths per 10-15 day clinical placement. The frequency of deaths during a clinical placement can also contribute to increased stress as there is often little time to process the death experience before continuing with end-of-life care for other patients.
Even though most students had previously experienced death, the findings highlight that the palliative care experience provoked feelings of sadness, anxiety and powerlessness. This feeling of powerlessness may relate to whether students' expectations of their capabilities and skills were too high. Such feelings of powerlessness have also been identified in other studies, but not fully explored in the context of palliative care (Parry, 2011). In response to how respondents felt during the clinical placement, no students reported the positive aspects of a palliative care placement, such as feelings of making a difference. This is an area that needs to be addressed further as part of palliative care education.
The notions of 'good death' and 'bad death' can also contribute to the experience and feelings of anxiety. In this study the nursing students' perceptions of the death experience are based on the support and care that can be provided during the death experience, and are linked to patient and family needs, effective communication, and symptom control. Dying in pain was a dominant element in participants' descriptions of a bad death. Students responded to the perceptions of death and dying from a broader perspective and not in the context of the clinical placement. It is reasonable to assume that the clinical placement experience would have also contributed to the responses. These findings are consistent with previous work by Wallace Grossman, Campbell, Robert, Lange, & Shea (2009); however, other more in-depth studies identified that nurses reported the importance of the maintenance of cultural practices and the need for supportive organisational resources to support the death process (Costello, 2006; Bradbury, 2000).
The nursing students reported feeling supported by the work environment and the various staff in the palliative care team, including volunteers, the chaplain and other non-nursing staff. The Practitioner Scholar was the person who was reported to have provided the most support. The findings indicate that the support provided for students was highly recognised and that, even though caring for a dying patient was stressful, the palliative care clinical experience was valued.
Debriefing is a specific form of support used as a teaching strategy in clinical placements. Debriefing can be used as part of everyday sessions in clinical settings and in specific situations such as after a patient death. In this study debriefing was identified as an important part of support following a death. While the Practitioner Scholar was reported as being the greatest support during experiences of death and dying, the findings revealed the multiple and varied members of the healthcare team provide support to nursing students in their care of dying patients. This may be due to the staff being experience in palliative care and as a result of the placement being located in a dedicated palliative care unit. Further exploration of how healthcare professionals are prepared to support and debrief colleagues and students following patient deaths may be valuable in encouraging and facilitating this role.
Previous experiences of debriefing, lack of opportunity for debriefing, and the interpretation of the concept of debriefing may impact on the value of debriefing. The study did not explore what other strategies students used to help manage their feelings of stress and sadness, but all students reported sharing experiences of death and dying with family, friends or fellow nursing students was helpful. Other studies have found that nurses do use informal support mechanisms and strategies to help them cope with the experience of a patient death (Rickerson, 2005).
The study findings demonstrate the value of dedicated palliative care education as part of preparation of students prior to clinical placements. Nursing students reported palliative care education prior to the placement contributed not only to their knowledge of palliative care `but also the environment and related expectations. The education sessions provided by the Practitioner Scholar during the clinical placement also further contributed to the development of knowledge and skills of palliative care. Other research has shown that palliative care education is critical to supporting students on placements and in the delivery of palliative care best practice (Barrere et al, 2008; Mallory, 2003).
This study highlighted the importance of palliative care clinical placements and the challenge to not only encourage graduate health professionals to enter into palliative care roles, but to have the knowledge and skills to deliver end-of-life care in any setting. The palliative care clinical placement provided students with knowledge, skills and practice to support palliative care, with two thirds of this nursing student cohort considering palliative care as a future work place. Further, the majority of students reported that the skills, knowledge and experiences gained during the palliative care clinical placement were transferrable to other clinical settings areas, and specifically the skills of communication with patients and families and pain management. As communication is fundamental to all nursing practice, the student recognition of this important aspect of nursing is very positive, and especially in view of the often challenging communication required in a palliative care setting.
Barrere, C., Durkin, A. & LaCoursiere, S. (2008). The influence of end-of-life education on attitudes of nursing students. International Journal of Nursing Education Scholarship, 5(1), 1-18. http://dx.doi.org/10.2202/1548-923X.1494
Chapman, R. & Orb, A. (2001). Coping strategies in clinical practice: The nursing students' lived experience. Contemporary Nurse: A Journal for the Australian Nursing Profession, 11(1), 95-102. http://www.contemporarynurse.com/archives/vol/11/issue/1/article/1717/coping-strategies-in-clinical-practice
Costello, J. (2006). Dying well: Nurses' experiences of 'good and bad' deaths in hospital. Journal of Advanced Nursing, 54(5), 594-601. http://dx.doi.org/10.1111/j.1365-2648.2006.03867.x
Davies, E. & Higginson, I. (2010). Delivering research in end-of-life care: Problems, pitfalls and future priorities. Palliative Medicine, 24(5), 456-461. http://dx.doi.org/10.1177/0269216310366064
Deffner, J. & Bell, S.K., (2005). Nurses' death anxiety, comfort level during communication with patients and families regarding death, and exposure to communication education: A quantitative study. Journal for Nurses in Staff Development, 21(1), 19-23. http://journals.lww.com/jnsdonline/Abstract/2005/01000/
Nurses__Death_Anxiety,_Comfort_Level_During.5.aspx
Dobbins, E. H. (2011). The impact of end-of-life curriculum content on the attitudes of associate degree nursing students toward death and care of the dying. Teaching and Learning in Nursing, 6(4), 159-166. http://dx.doi.org/10.1016/j.teln.2011.04.002
Hopkinson, J., Hallett, C. & Luker, K. (2005). Everyday death: How do nurses cope with caring for dying people in hospital? International Journal of Nursing Studies, 42(2), 125-133. http://dx.doi.org/10.1016/j.ijnurstu.2004.06.004
Kent, B., Anderson, A. & Owens, R. (2012). Nurses early experiences with patient death: The results of an on-line survey of Registered Nurses in New Zealand. International Journal of Nursing Studies, 49(10), 1255-1265. http://dx.doi.org/10.1016/j.ijnurstu.2012.04.005
Kurz, J. M. & Hayes, E. R. (2006). End of life issues action: Impact of education. International Journal of Nursing Education Scholarship, 3(1), 1-11. http://dx.doi.org/10.2202/1548-923X.1189
Malloy, P., Paice, J., Virani, R., Ferrell, B. & Bednash, G. (2008). End-of-life Nursing Education Consortium: 5 years of educating graduate nursing faculty in excellent palliative care. Journal of Professional Nursing, 24(6), 352-357. http://dx.doi.org/10.1016/j.profnurs.2008.06.001
Meraviglia, M., McGuire, C. & Chesley, C. (2003). Nurses' needs for education on cancer and end-of-life care. The Journal of Continuing Education in Nursing, 34(3),122-127.
Mok, E. & Chiu, P. C. (2004). Nurse-patient relationships in palliative care. Journal of Advanced Nursing, 48(5), 475-483. http://dx.doi.org/10.1111/j.1365-2648.2004.03230.x
Mok, E., Wai & Kam-yuet, F. (2002). The issue of death and dying: Employing problem based learning in nursing education. Nurse Education Today, 22(4), 319-329. http://dx.doi.org/10.1054/nedt.2001.0708
Parry, M. (2011). Student nurses' experience of their first death in clinical practice. International Journal of Palliative Nursing, 17(9), 448-453. http://www.internurse.com/cgi-bin/go.pl/library/abstract.html?uid=86569
Rickerson. E., Somers, C., Allen, C., Lewis, B., Strumpf, N. & Casarett, D. (2005). How well are we caring for caregivers? Prevalence of grief related symptoms and need for bereavement support among long term care staff. Journal of Pain and Symptom Management, 30(3), 227-233. http://dx.doi.org/10.1016/j.jpainsymman.2005.04.005
Seymour, J., Gott, M., Bellamy, G., Ahmedzai, S. & Clark, D. (2004). Planning for end of life: The views of older people about advance care statements. Social Science & Medicine, 59(1), 57-68. http://dx.doi.org/10.1016/j.socscimed.2003.10.005
Wallace, M., Grossman, S., Campbell, S., Robert, T., Lange, S. & Shea, J. (2009). Integration of end-of-life care content in undergraduate nursing curricula: Student knowledge and perceptions. Journal of Professional Nursing, 25(1), 50-56. http://dx.doi.org/10.1016/j.profnurs.2008.08.003
| Please cite as: Gallagher, O, Saunders, R., Tambree, K., Alliex, S., Monterosso, L. & Naglazas, Y. (2014). Nursing student experiences of death and dying during a palliative care clinical placement: Teaching and learning implications. In Transformative, innovative and engaging. Proceedings of the 23rd Annual Teaching Learning Forum, 30-31 January 2014. Perth: The University of Western Australia. http://ctl.curtin.edu.au/professional_development/conferences/tlf/tlf2014/refereed/gallagher.html |
© Copyright 2014 Olivia Gallagher, Rosemary Saunders, Karen Tambree, Selma Alliex, Leanne Monterosso and Y. Naglazas. The authors assign to the TL Forum and not for profit educational institutions a non-exclusive licence to reproduce this article for personal use or for institutional teaching and learning purposes, in any format, provided that the article is used and cited in accordance with the usual academic conventions.